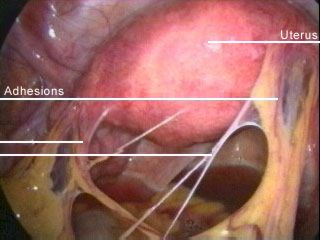
Surgical methods to minimise adhesions
Reducing adhesions during surgery for endometriosis has improved greatly with new surgical techniques.
Some of these new surgical methods will be of value to discuss with your surgeon prior to treatment, to assess whether your surgeon has up to date information of these new techniques.
Being able to reduce the formation of adhesions is a big development in surgical treatment, and is also a huge benefit to assist in successful healing and better chances of conception after surgery.
One of the most common treatments for endometriosis is through surgery with a procedure called a laparoscopy (allowing the surgeon to have a visual look at the organs in the abdominal cavity).
During the surgery the growths of endometriosis are removed, along with any cysts. Unfortunately any type of surgery can lead to scarring and adhesions where organs can stick together. Usually these develop because there is scar tissue in the pelvic region in the sites and locations that the surgeon has removed any endometriosis.
This scar tissue can easily fuse to other organs in the pelvic region that it touches as it heals. Also adhesions can develop in the abdomen/pelvic cavity where two areas of endometriosis come into contact. This is more common with more advanced endometriosis.
Prevention of adhesions
The best way to prevent adhesions is through experienced surgical techniques, and a surgical method that minimises tissue injury and heavy bleeding. It is important to prevent blood loss at the site of any surgery, since excessive abdominal bleeding increases the likelihood of adhesions.
Surgical barrier agents
There are various types of barrier agents which can be used to reduce the risk the growth of adhesions, which include non-absorbent barriers, absorbable barriers and fluids. Each of these methods work by separating damaged tissue during the healing process.
One barrier product that is used is Interceed which is an absorbable barrier which is made from regenerated cellulose. It is a mesh which does not require suturing, and it is draped over the injured tissue and within an eight hour period it forms a gelatinous protective layer which is absorbed into the body in about two weeks. Interceed has reduced adhesion formation by 50 percent.
Another product that is used is Seprafilm, which is an absorbable membrane that becomes a hydrated gel within 24 hours of placement and is absorbed into the body within seven days. This product has been very effective in reducing adhesions in abdominal surgery.
New surgical techniques
There are now new surgical techniques that have been developed which can help to minimise this problem from developing.
A new product called Spraygel is currently being tested in the United States. It consists of two liquids that are mixed during spraying, and when mixed they form an absorbable hydrogel.
This fluid adheres and remains intact for five to seven days and then it is absorbed and excreted. It is reported that this product has decreased the frequency and amount of adhesions by 70 percent.
Adhesions causing the need for further surgery
Many women with endometriosis have had to undergo further surgery simply to remove the adhesions caused by previous surgery. It is estimated that 10 to 15% of women require repeat surgery for this reason. Therefore, if the surgeon can minimise the potential risk in the first place, then the healing process that follows is much better.
Before having surgery ask your surgeon if they are using these new techniques to help reduce the possibility of future adhesions.

About the Author
Hi, I am Carolyn Levett, the Founder here at endo-resolved - I am an Integrative Health Coach having studied nutrition, naturopathy and aromatherapy as well as being a published author of three endometriosis books. I used to suffer from severe endometriosis and was fortunate to be able to regained my health and recover from this disease with the support of nutrition, natural therapies and lots of determination.
My motivation is to help other women with endometriosis to heal their bodies so they may start to overcome this awful disease without having to totally rely on toxic drugs and surgeries which can cause further damage - with healing thoughts, Carolyn.
 As featured in
As featured inReferences:
New surgical methods prevent adhesions - Pubmed
Interceed use to reduce post operative adhesions - Pubmed
Seprafilm adhesion barrier post surgery - Pubmed